It’s very easy to feel like a small cog in the big wheel of health and social care. ‘When things aren’t right, how can I fix it?’
We have just finished writing a new on-line course ‘A Change in Behaviour’ and I was given the opportunity to design a module looking at the role of institutions and how they influence how people are controlled and how they react to institutional control.
Institutions are impossible to avoid, whether they are tangible (such as schools, hospitals or prisons) or exist in our collective minds (marriage, religion). They help to hold our society together and are seen as having a big role in protecting people.
Institutions have power and can make humans behave in unexpected ways. Philip Zimbardo the American Psychologist wrote: ‘When placed in an extreme environment, one tends to assume that their values and morals can overcome the harsh situations in that environment.’
His observations and experiments and those of his mentor Stanley Milgram seemed to show that; ‘Our roles in social institutions have a huge influence on our behaviours, attitudes and beliefs. When placed in an extreme environment, individuals usually begin to stress and feel unsafe. When assigned to authoritative roles, individuals in toxic environments tend to act aggressive and arbitrarily.’
Social identity theorists argue that when in a group, we experience a shift from our individual selves to a collective self, and our behaviour in response to this shift is regulated by the social norms shared by our fellow group members.
The power of the institution is so strong and overwhelming, and it is easy to understand how people may feel compelled to adjust their behaviour to ‘fit in’.
The response to these phenomena seems often to be reactionary. When institutions fail it comes at a huge cost to individuals. People experience abuse and harm, the people bringing the abuse to light often experience harm, denial and harassment too.
Legislation, standards and recommendations can only ever take us so far in making things right. The underlying culture remains.
No one individual can fix a failing institution. Often; ‘The response to abuse is for the dementia care community to press for more staff, training and skills. The prevailing belief seems to be that if everybody was well trained in dementia care mapping or reminiscence or validation, then maybe our trouble with poor quality care would be at an end.’ Paul Whitby
I think that’s true, and the interventions miss the point. It’s about cultural and behavioural change. Teams within institutions themselves need to set the ground to enable people to tackle institutional abuse. We need more proactive honesty, collectively as teams.
Think about the organisation you work for or know well. Where do you think the organisation is on accepting the following?
- Whilst approaches to supporting people living with dementia have changed, institutions by their very nature are slow to adapt
- Institutions despite the best intentions of working within it can be impersonal with a one-size fits all approach
- Systems and routines developed over many years by institutions can be seen to become more important than the people they were designed to support
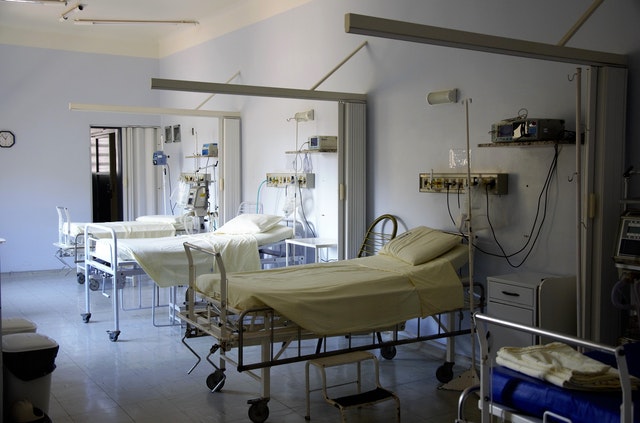
- Environmental features in most care institutions disable rather than enable people living with a dementia
- Large institutions because of their history, power and resources can make people feel small (alienated) and powerless when they need to challenge outdated and potentially abuse ways of working.
We can never assume that our values and morals alone can overcome a harsh situation in an environment.

Consultant Learning & Development Manager
MCM
References
Milgram. Stanley (1974). “Obedience to Authority: An Experimental View”. 2010. Pinter and Martin Ltd
Social Identity Theory – an overview | ScienceDirect Topics
Paul Whitby (2008) Why is a good quality residential care so very difficult to achieve?
Journal of Dementia Care. Hawker Publications